What’s in store for MedEd? An interview with Dr. Brigham Willis
April 29, 2022

We sat down with Dr. Brigham Willis, Founding Dean of the University of Texas at Tyler School of Medicine (UT Tyler), to get his thoughts on the emerging trends in MedEd and how medical schools are adapting to change. Read what he had to say.
Q: What do you think are the major trends shaping MedEd right now and over the next few years?
A: I think everyone is noticing and talking about the shift from passive to active learning to encourage student agency. This is vastly different from my days as a medical student; most of the time was spent in a classroom listening to lectures, but not really learning all that much, and we’d just go home and relearn the material anyway.
Students today are savvy. They can access facts in so many different places on their own. We also need to recognize that facts change all the time, and medical knowledge is only increasing. It’s not practical to try to cram in all these facts, when we can spend more time teaching students how to think, building their empathy and humanism, and preparing them for real clinical experiences and patient interactions. Basically, what I’m saying is that we’re beginning to change the way we teach.
Q: How has this impacted your school of medicine, and what opportunities do you see there for your team and students?
A: Actually, one of the reasons I was so excited to join UT Tyler was their innovative approach to teaching. They designed an entirely flipped classroom. There are almost 0 lecture hours because everything is asynchronous. For example, students are given a menu of things to learn on their own. If they’re learning about cardiovascular physiology, they’re given a bunch of resources to study in advance. When they do come to class, which is only for about 20 hours a week, that time is spent working through cases or problems as a group based on what they’ve learned. That is then extended to the anatomy lab where they get that tactile learning experience and even conduct an ultrasound to see physiology in action. It’s all authentic and high fidelity, and gives students agency in how they learn.
This model works and newer medical schools like UT Tyler are able to quickly embrace it. This transition is understandably harder for older medical schools to make, but it’s important enough that many of these schools have task forces and working groups dedicated to this issue.
Q: There has been a lot of focus on the challenging transition from UME to GME. Are there any promising initiatives you think schools should keep an eye on?
A: I think what’s helped over the last few years is earlier clinical experiences in medical school. Students are way more comfortable in clinical situations now than when I went to school. But, there’s still a big step up in workload that needs to be addressed. Some of that has to do with the focus on protecting medical students’ wellness. I remember doing 80 to 90 Duty Hours per week as a medical student, which you don’t see anymore. I think that’s a good thing because burnout is a major problem. We have to do what we can to reduce burnout in residency, but in a way that still ensures students are ready for the demands of residency and get the necessary hours under their belt to become an expert in their clinical field.
I think striking that balance between reduced work hours with purposeful learning activities can help ease that transition. Let’s say you’re on a surgery rotation. Instead of waiting countless hours for a random patient to come in to hopefully gain that experience, you could easily gain that experience through high-yield learning activities such as simulations and virtual reality. It’s faster and more efficient.
Q: Your emphasis on the learning model aligns with what we’ve been talking about at Acuity, which is Precision Medical Education — using advanced analytics to individualize training. How do you think this concept can help improve learner outcomes?
A: Well, I think it’s evident that data can help a lot. I’m actually working on a paper right now about quantifying resident experience and individualizing their training based on gaps we can see. For example, if we look at EMR data, compare each resident to their class, and see that they didn’t do enough developmental assessments, we can send them to a developmental clinic to get that experience. This allows us to be responsive to a resident’s specific learning needs at the right time. At the end of the day, no one is the same, so we can’t use a one-size-fits-all instruction model. Data can help us make evidence-based and tailored decisions for each resident. Doing that ultimately builds their competence, which in turn boosts their confidence — and gives them more wellness time. I see it as a win-win-win. The challenge is getting there, but we have some of that foundation in place.
Q: So what role can a MedEd partner like Acuity do to support these changes in medical schools you’re talking about?
A: I think something that Acuity already provides with its software is a clear picture of vertical and horizontal integration and gap and redundancy analyses. These types of tools are critical. I also think products that allow schools to better track individual students through their whole course in a real-time, comprehensive dashboard can help advisors coach them and take early intervention, if needed. It’s really all about boosting learner outcomes.
Related Articles

How interviews could be misleading your admissions...
Most schools consider the interview an important portion of their admissions process, hence a considerable…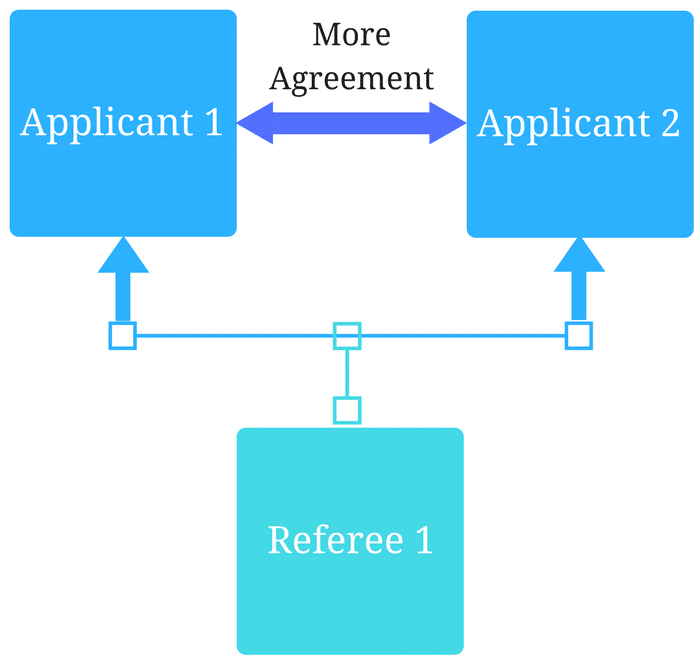
Reference letters in academic admissions: useful o...
Because of the lack of innovation, there are often few opportunities to examine current legacy…
